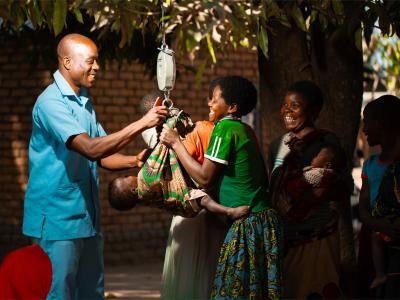article / October 10, 2025
Deworming Campaign Boosts The Health Of 85,000 Children In Mozambique
A partnership between the Ministry of Health and the Consortium led by World Vision, the Partnering for Sustainable Education Outcomes (PARES) project conducted a deworming campaign that benefited over 85.000 children in Nampula and Zambezia provinces in northern and central regions of Mozambique.
press release / October 2, 2025
World Vision International Lao PDR and Ministry of Health Extend Deworming Program for Children Under Five
World Vision and Lao Ministry of Health Partner Again to Deliver 800,000 Deworming Tablets for Young Children
publication / February 6, 2026
World Vision Haiti Annual Report 2025
World Vision Haiti’s annual impact report highlights how we protect children, respond to crisis, and build resilience in vulnerable communities.
article / January 21, 2026
Southern Province Chiefs Join Efforts to Improve Maternal and Child Health
Traditional leaders across the Southern Province are collaborating with health partners to enhance the nutrition of pregnant women and safeguard the health of their babies. This comes at a time when maternal nutrition remains a concern. The 2024 Zambia Demographic and Health Survey shows that anaemia affects about one in five women of reproductive age. The survey also highlights ongoing micronutrient deficiencies among women and children, especially in rural areas. Poor nutrition during pregnancy increases the risk of illness for mothers and affects a child’s growth from the very beginning. These findings show why practical solutions and strong partnerships at the community level are needed.
article / November 18, 2025
Vitamin A and Albendazole Gifts-in-Kind (GIKs) Donated to Health Ministry
World Vision Eswatini, through its Gifts-in-Kind (GIKs) Programme, has handed over 48,000 tablets of Vitamin A and 24,000 Albendazole in 400mg to the Ministry of Health in support of the country’s efforts towards improved health for children and in line with the organisation's ENOUGH Campaign to End Child Hunger and Malnutrition.
article / November 18, 2025
A Fight Against Malnutrition: How the Zambia Multiple Micronutrient Supplementation Project is Changing Lives in Mbala
Recent data from the 2024 Zambia Demographic and Health Survey paints a troubling picture: over a third of children under five are stunted, and nearly half of pregnant women suffer from anaemia. These alarming figures reveal a harsh reality: malnutrition and poor maternal health are severely affecting communities across Zambia, especially in communities like Mbala.
article / February 19, 2026
World Vision’s Integrated Programs Transform Learning, Health, and Hope for 1,052 Learners in Pitseng
World Vision’s integrated programs transformed a primary school in Pitseng, providing clean water, safe toilets, new classrooms, school gardens, and poultry projects, improving learning, hygiene, and student wellbeing
article / March 6, 2026
Bridging the Gap: Clean Water as a Foundation for Health and Education in Mwinilunga
On February 18, 2026, Sailung’a Health Facility in Mwinilunga District marked a major step toward improved health services. World Vision Zambia handed over a modern ablution block and water system to the facility. The new infrastructure strengthens access to safe water and sanitation for patients, mothers, children, and health workers.
video / March 4, 2026
Partnerships for Progress: Strengthening Rural Health Through Collaboration
In this video, World Vision’s Vice President for Water and Health highlights the transformative power of partnerships in bridging the gap between remote communities and quality healthcare. While WASH services provide the foundation for safety, strategic collaborations bring the specialised resources necessary to sustain a modern medical environment. By aligning the expertise of non-profits with the strengths of the private sector, rural health infrastructure is upgraded from basic survival centres to comprehensive medical hubs capable of delivering long-term impact.
article / February 10, 2026
Community Health Clinics Improve Access to Quality Healthcare in Mposa
Village Health Clinics in Mposa, Malawi, are saving lives by bringing healthcare closer to mothers and children. With support from World Vision, trained Health Surveillance Assistants now provide critical care, reducing illnesses like pneumonia and diarrhea. Mothers like Hadija Biliati no longer face long journeys for treatment, and child health outcomes are improving.