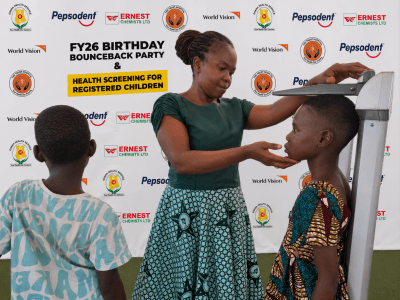publication / May 13, 2026
World Vision Southern Africa Region Health & Nutrition Capacity Statement
Explore World Vision Southern Africa Region’s 2025 health and nutrition impact across Southern Africa, reaching 3.6 million people through community health systems.
video / May 11, 2026
Frontline Defenders: Community Health Workers Determined To End Malaria
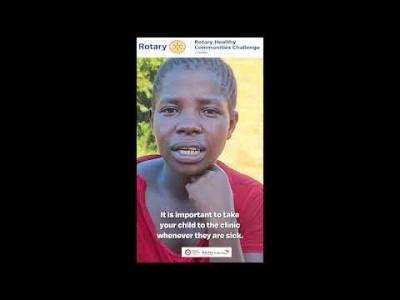
World Vision Zambia's volunteers are more determined than ever. Every day, they show up on the frontlines, providing treatment and health education to fight Malaria, Pneumonia, and Diarrhoea in communities across Zambia under the Rotary Health Communities Challenge.
video / May 11, 2026
No More Mothers Should Grieve: World Vision Zambia's Fight Against Malaria
"I lost my child at only eight months to malaria. The pain of losing a child to a preventable and treatable disease is devastating," recalls Felistus, a mother from Zambia.
Felistus's story is one of many that reflect a harsh reality facing families across the country, children dying from diseases that do not have to be fatal.
publication / May 14, 2026
Community Health Workers Capacity Statement
World Vision’s Community Health Workers Capacity Statement highlights global impact, evidence, and systems support across 43 countries.
article / April 30, 2026
Reversing the Rise: Community-Led Action Against Malaria in Mozambique
Discover how community mobilization and Seasonal Malaria Chemoprevention are transforming malaria prevention in Tete, Mozambique, protecting children and strengthening trust in health services.
publication / May 11, 2026
Southern Africa Region Health and Nutrition Capacity Statement
World Vision SAR delivers health and nutrition services at scale, strengthening community health systems and improving outcomes across Southern Africa.
publication / May 4, 2026
World Vision’s Health and Nutrition Capacity Statement
Discover how World Vision improves health and nutrition across East Africa through community-based care, malnutrition treatment, and maternal and child health services that save lives.
article / May 6, 2026
Rehabilitating Care: A Renewed Health Centre for All
After conflict-related damage forced the Derdghaya Socio-Medical Centre to close, World Vision and the Imam Sadr Foundation rehabilitated the facility, restoring vital healthcare services for thousands of people across South Lebanon.
article / May 11, 2026
Community Voices Drive Change at Kasikili Health Post
Kasikili Health Post sits on the outskirts of Pemba District, approximately 22 kilometres from the District Health Office. It serves a catchment population of around 6,875 residents, providing essential primary healthcare to families across the area.
article / May 1, 2026
World Vision Ghana Organises Health Screening for Children in Agotime-Ziope District
World Vision Ghana organised free health screening for children in the Agotime-Ziope District.