publication / February 4, 2026
East Africa Region Policy Brief on Ending Female Genital Mutilation (FGM) 2023
World Vision is influencing the adoption and implementation of policies relating to FGM in Kenya, Sudan, Somalia and Sudan. The policy brief highlights strategic policy recommendations targeting national governments, regional institutions donors faith and community leaders.
publication / January 5, 2026
World Vision Ghana Newsletter - Edition December 2025
Discover how World Vision Ghana is driving transformation despite challenges. From education and health to WASH and child protection, our latest newsletter highlights progress, resilience, and partnerships that ensure every child thrives.
article / December 24, 2025
Building something of our own – how a small-scale business support led to a new beginning
Satrudhan once struggled to make ends meet and care for his child with a disability. With World Vision’s business support, they now thrive and dream big in Nepal.
publication / March 4, 2026
COMPOUNDING RETURNS: A Study On Remittance Loss and The Cost Of Deportations in Afghanistan
The study shows deportation is an economic and protection shock that reverberates through households and local markets. Deportation removes income earners from foreign labour markets, abruptly cutting off remittance flows. This loss of income translates into debt accumulation and asset depletion as households struggle to meet basic needs. Growing indebtedness then drives harmful coping strategies and distress practices.
publication / September 12, 2025
Measuring the Experience of God's Love
Research on how children experience God’s love, showing hope as a key sign of spiritual well-being across cultures and contexts.
publication / September 3, 2025
Behaviour Change: Evidence Summary for Food Hygiene
Food hygiene is critical to health, with 600 million people falling ill annually due to contaminated food. Children under five bear 40% of the burden, with 125,000 deaths each year.
publication / August 19, 2025
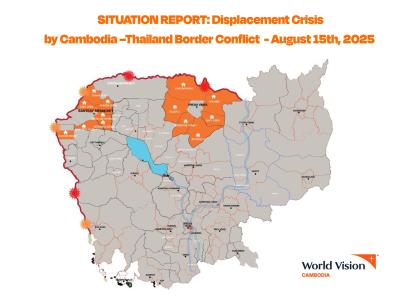
Situation Report: Displacement Caused by Cambodia –Thailand Border Conflict - August 15th, 2025
World Vision International in Cambodia (WVI-C) has activated a Category I National Emergency
Response to address the humanitarian needs resulting from the Cambodia-Thailand border conflict.
Our immediate intervention focuses WASH, education, child protection, food and non-food items to
56 safety centers with 11,727 families, comprising of 51,236 individuals (35,506 adults and elderly
and 15,730 children), in Preah Vihear, Banteay Meanchey, and Siem Reap.
publication / July 2, 2025
ODA at the crossroads
Child-focused aid is shrinking despite rising global crises. Investing in children is urgent, smart, and essential for a stable, equitable future.
publication / March 13, 2025
Cash Waves Report: Executive Summary
This research, commissioned by World Vision’s Middle East and Eastern Europe (MEER) regional office in partnership with Qualisus Consulting, aims to assess the broader impact of cash and voucher assistance (CVA) programmes on marginalised groups and young people’s mental health and psychosocial well-being, livelihood-resilience, community and social cohesion, and child well-being.