press release / May 18, 2026
DR Congo: A New Ebola Variant Declared in Ituri Threatens Children’s Lives
This press release highlights the declaration of the 17th Ebola outbreak by the Democratic Republic of Congo in Ituri province. This new outbreak is the Bundibugyo variant, which does not have any treatment or vaccines, making the response most complex. It is also spreading rapidly as the province of North Kivu has declared one confirmed case, and Uganda has confirmed 1 case. World Vision is calling for a coordinated and cross-border response.
publication / May 19, 2026
Capacity Statement: World Vision's Livelihoods and Economic Recovery Approach in Ukraine
World Vision Ukraine's Capacity Statement: How we drive economic recovery and livelihood support to help 1M+ people transition from relief to resilience.
video / May 19, 2026
The Power of Early Nutrition Support - WVSR nutrition project in Syria
After months of worry about her daughter’s health, a mother in Syria finally began to see hope. Through nutrition support provided by World Vision Syria Response and health facilities supported across Syria, her daughter received regular follow-ups, nutritional supplements, and care that helped improve her health step by step.
Today, her smile is a reminder of the life-changing impact of early nutrition support.
article / April 24, 2026
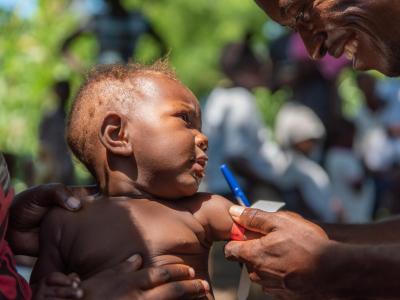
10 Facts about Vaccination
Vaccinations are life-changing for children and communities living in the world’s toughest places. Here are 10 facts
page / April 22, 2016
Intervention 10: Prevention, care seeking and treatment for pediatric HIV
Prevention, care seeking and treatment for pediatric HIV (including ARVs and cotrimoxazole prophylaxis) Children and youth compose an undeserved key population in the struggle against HIV.
publication / March 18, 2021
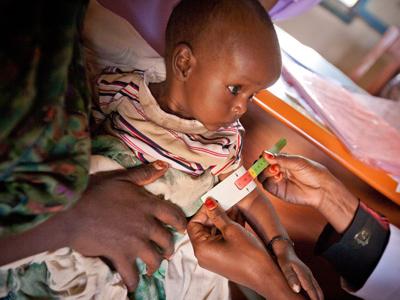
Using community volunteers to deliver treatment for acute malnutrition
This presentation on using Community Health Worker to deliver treatments services for acute malnutrition in Angola was given at a Severe Acute Malnutrition conference.
article / September 27, 2024
Aid in health centers goes beyond treatment
“With the support of World Vision and Medair, the clinic became an important hub for food and medical assistance” – Hadi, health facility manager.
publication / February 6, 2018
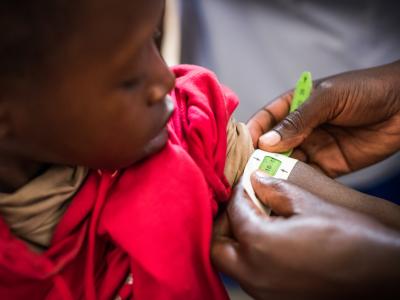
Community-based Management of Acute Malnutrition
Community-Based Management of Acute Malnutrition (CMAM) is a decentralised community-based approach to treating acute malnutrition. Treatment is matched to the nutritional and clinical needs of the child, with the majority children receiving treatment at home using ready-to-use foods.
article / May 10, 2024
A life changing intervention program for reducing malnutrition in Zimbabwe
Expressing her heartfelt appreciation, Mrs. Chimbu extends her thanks to USAID, World Vision Zimbabwe, and the MSASA project for making this life-changing program a reality.