Malawi: Fighting malaria in the midst of COVID-19
Among Malawians, Balaka is a storied town on a hill. It is a district that has kept on giving - music that has withstood seasons and inspired generations.
But still, all is not rosy in this citadel of music. Just opposite the St. Louis Church, where some of the Balaka music Malawians enjoy was born and perfected, Balaka District Hospital is stretched.
Just outside the hospital, it is a busy day. A steady throb from the stereos of battered public motorbikes is making noise as they bring patients from different parts of the district. Of course, the skies have just birthed the sun, it is hot, and many are thirsty. Home-made low-cost plastic packs of water are widely being sold.
Deep inside the hospital, the sound of infants crying, machines beeping and nurses pushing trolleys fill the ward.
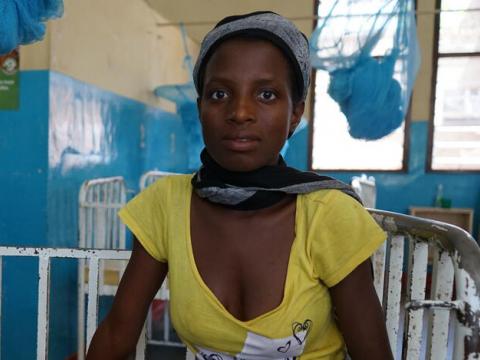
In a sweltering room in the corner of the emergency children’s ward, Melise is restless.
Cradling her two-year-old son, the 18 year old is a picture of focus in the children’s ward. Her child, Gracian, cried a lot last night. They did not sleep. Gracian is sick. He is fighting malaria.
Over the past decade and a half, the level of infant mortality in Malawi has significantly dropped and raised hope among many.

The under-five mortality rate fell from 74 deaths for every 1,000 live births in 2008/9, to 52 deaths for every 1,000 live births in 2014. But malaria has remained a constant battle.
Amid this progress, in Balaka and other districts, malaria is still an issue, especially for the two most at-risk groups - children and pregnant women.
Melise sits on the edge of bed helpless, watching over her son Gracian. He has just finished a drip, his fifth since being admitted for malaria some three days ago.
“Today he is a bit better,” says Melise. “I hope he keeps improving so we can be discharged.”
Melise gives a sign to another guardian, three beds away, to watch over Gracian. She is thirsty. She goes out to find water and returns less than five minutes later.
Close to the ward entrance, four nurses are putting together their gear for another round of treatments in the ward.
Apart from Gracian, Melise is equally concerned about home. She left a basketful of tomatoes that she had just procured to resell at her local market.
“There’s no one to sell them for me,” she says as she tries to caress her son to sleep after a night on the drip without sleep.
Since they were ripe when she left, Melise believes most of the tomatoes will now have gone bad.

With 71% of Malawians living in the economic periphery, spending less than US$1.90 a day, the daily economic losses, compounded by high household costs associated with malaria treatment, constitute a major economic burden for the underprivileged.
Just seven months ago, Gracian was hospitalised due to malaria, Melise had to transport costs to get to the hospital. She is consistently thrown into the depths of poverty by malaria. Unfortunately, that’s the tale for many in Balaka district.
“Towards the end of 2018, we distributed long-lasting insecticide-treated nets to fight malaria, but there was no significant change,” says the District Environmental Health Officer for Balaka, John Mawaya.
“Most of our health workers in Balaka spend much time fighting malaria. It is expensive for the families of the sick and for us as a department,” adds Mawaya.
A report published by the Malaria journal in 2017 reports that “total household costs averaged US$17.48 per patient; direct and indirect household costs averaged US$7.59 and US$9.90, respectively” when treating malaria.
the bulk of these costs are driven by facility management, the patient's distance from a health facility, the age of the patient and the duration of their hospital stay.
Because of women like Melise, World Vision’s Prince Nkhata, Deputy Chief of party for World Vision’s malaria interventions in Malawi, appeals to development partners to do more to eradicate malaria - not just to save the resources the country spends on treating the disease, but to allow people to have time to improve their livelihoods.
“If you try to think of how many people are admitted for malaria today, or those being nursed from home, and the people providing that particular care, you’ll realise that we cannot develop as a nation if we do not tackle the burden of malaria,” Nkhata says.

“We need to dig deep in our efforts to fight malaria, because by doing that, we will ease pressure on our health facilities, save resources, and ensure that our healthy population is working hard and participating in the economy,” reiterates Chikonga.
“Malaria causes most of the hospital admissions and even tops diseases treated for outpatients. Our HSAs and clinicians spend most of their time educating people about malaria and treating it, which takes their time away from other diseases,” Mawaya notes.
World Vision and the Malawi Government, with financial support from the Global Fund, has sprayed over 132,000 houses in Balaka district, and Melise is among the beneficiaries.
Melise is intrigued with the idea being safe from malaria. “Of course, we can always get sick, but if we can be free from malaria, and spend time at home, our lives may improve,” she says.
Similar exercises have been held in Mangochi and Nkhatabay districts, where 351,000 and 67,000 houses respectively have been sprayed. Across the three districts, over three million people have been safeguarded from malaria.
Concerted efforts by agencies, including the Global Fund and the US Government’s Presidential Initiative, have contributed to a global reduction in malaria mortality rates. According to a 2020 report by the World Health Organisation, over the period 2000-2019, malaria-induced deaths fell from 736,000 in 2000 to 409,000 in 2019.
The percentage of total malaria deaths among children aged under 5 years was 84% in 2000 and 67% in 2019.
By Charles Kabena, Communications and External Engagement Manager.