Breastmilk, the perfect first food for newborns for at least six months

When the 23-year-old Esther Anyango started feeling uncomfortable, she told her husband who dashed her to the nearby health facility for medical attention. Little did she know she was due to birth to twins. At only seven months, the twins—Edwin and Eunice—were born. “I had fully done all my antenatal care visits required of an expectant mother,” says Esther who earlier had had two normal deliveries at full term without any complication. “I didn’t have any bad signs. So, I was taken aback when the midwife asked me to go to the delivery room.”
Esther gave birth to her twins in September 2020 at Lunyo Health Centre III in Busia district, which was fully reconstructed and equipped with support from World Vision. And, with the training of medical staff, Brenda had safe labour and delivery. “It was a joy to give birth at the hospital that has clean water and where I could clean myself and the babies after giving birth,” says Esther. “I felt safe and cared for by the staff, and the experience was a good one.”
Born before the end of the full term of gestation, the twins were tiny and weighed far less than normal children. But the mother of four says that she loved them at first sight—and that love continues to blossom. “My twins are so special,” she says with a chuckle kissing her twins. “They were born too early, too tiny, but we thank God because each passing day is a miracle in our life. My twins are the evidence of God’s mercy and grace.”
That is not all. Esther and her husband, Rogers Ouma have earned themselves special titles—Nnalongo and Ssalongo—in their community, courtesy of the twins. “Whenever I am called Nnalango I feel I am on the top of the moon,” says Esther. “It just feels so nice as it’s a sign of respect.” Among the Bantu people in Uganda, Nnalongo and Ssalango are revered titles given to the mother and father of twins respectively.
At the health facility, Esther was helped to take care of her twins using the Kangaroo Mother Care technique, where a mother from the hour of delivery holds a baby skin-to-skin for one hour a day. She was also reminded of the importance of exclusive breastfeeding for at least six months.
World Vision through the AIM Health Plus project, trained and supported more than 230 lead mothers—community health volunteers—to boost awareness among families and communities about healthy and safe feeding practices for young children as well as promoting health-seeking behaviour. “We focus on improving nutrition during the critical period from a mother’s pregnancy until her child is two years old,” says Mildred Orishaba, AIM Health project manager. “Working with community health workers, we educate mothers [on] optimal and safe feeding practices, and mothers learn how to keep their young children healthy and well-nourished.”
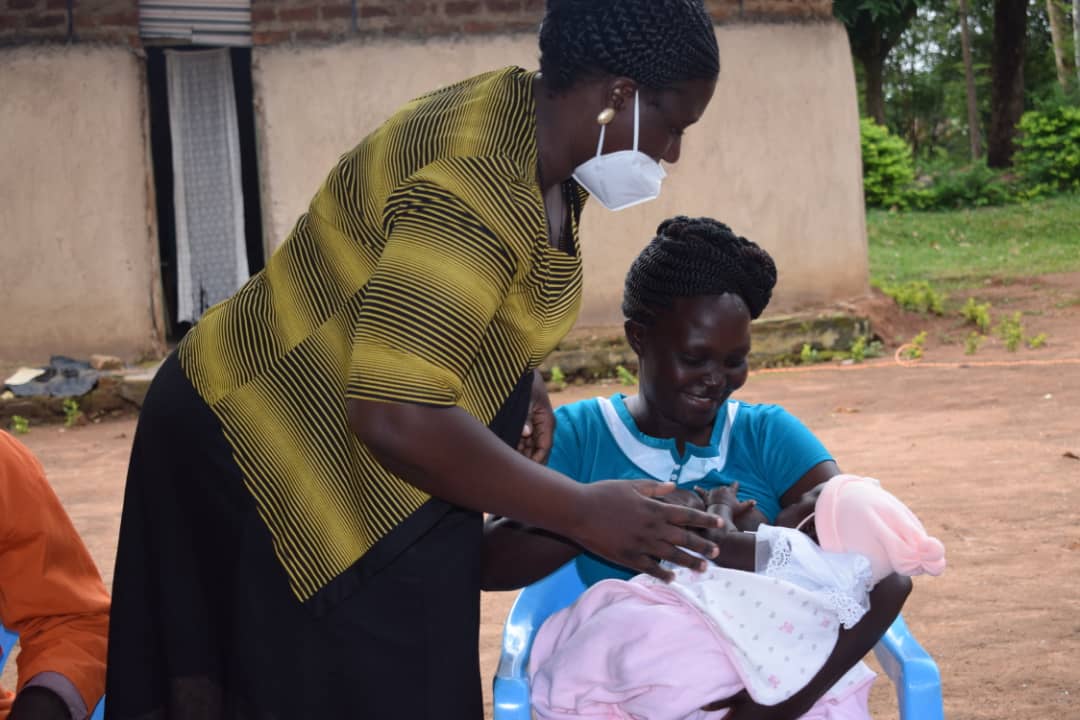
In the rural community of Lunyo, Esther proudly shows off her big baby twins at a health facility where she has brought them for a regular check-up, and to listen to health workers on how best to care for them. With their chubby legs and broad cheeks, Edwin and Eunice are a picture of good health and strength. Esther knows why: She has faithfully breastfed the children since they were born, thanks to the advice and encouragement from her community health workers.
Esther comes from a community where mothers frequently delay breastfeeding and prematurely introduce liquid and other solid foods, a practice, according to health experts, puts babies at risk of illness, stunted growth, and death.
Moreover, the World Health Organisation (WHO) recommends exclusive breastfeeding for the first six months of life, meaning the infant should only receive breastmilk without any additional food or drink – not even water – apart from syrups and medicines for a half year. The breastfeeding should be as often as the child wants, both day and night. WHO further recommends colostrum (the yellowish sticky breastmilk produced at the end of pregnancy) as the perfect first food for the newborn.
Evidence shows that breastfeeding provides the critical nutrients, antibodies, and fluids babies need to stay healthy and to develop sensory and cognitive abilities. But available statistics paint a dismal picture. According to the 2016 Uganda Demographic Health Survey, only six in 10 Ugandan children below the age of six months are exclusively breastfed.
What’s more, only six in 10 mothers initiate their babies breastfeeding within an hour of giving birth. A slight improvement was recorded from 63% in 2011 to 66% in 2016. It is no wonder then that the under-five and infant mortality rates stand at 64 and 43 per 1,000 live births respectively, which is very high by developing world standards.
This widespread cultural practice is what makes the day’s topic – exclusive breastfeeding – a special one to mothers like Esther. A few weeks after Esther became pregnant with twins, she spoke with a lead mother who told her about nutrition and caring for the pregnancy. The lead mother also talked to her about HIV counselling and testing, the benefits of giving birth at a health facility, and options for planning her births, including exclusive breastfeeding as a natural family planning method.
“It was our lead mothers who opened my eyes about breastmilk,” Esther says. “They always visit, counsel, and encourage us to have nutrition gardens to ensure we are healthy and strong for the time of delivery and [have] enough breastmilk for our babies. I had six prenatal care visits to learn more about what to expect during and after delivery.”
A browse through the medical records for Edwin and Eunice shows they are healthy. “Twin’s height and weight are normal, and they are lively,” says Donatia Erumbi, a midwife at Lunyo Health Centre III in Busia district. “They’re strong, their faces are rosy, and their breathing is normal, so I must commend and encourage their mother to continue with exclusive breastfeeding.”
Now, Esther describes how strong and healthy her baby twins are, and shares what she learns with new mothers in her care group—Ahusakanya—that meets twice every month. During these sessions, mothers share experiences to help themselves overcome the cultural barriers to early and exclusive breastfeeding—and to ensure every baby has a chance to grow up healthy and strong. “When I look at my boy and girl,” says Esther. “I’m convinced that they’ll live a healthy, happy life because I’m giving them the best start with breastmilk. That’s my wish for every child in my community.”
The Ireland-funded project was designed to improve the nutritional status of children under 5, and pregnant and breastfeeding mothers across 16 communities in the district of Busia in Eastern Uganda. AIM Health Project also aimed at increasing access to, and use of maternal and child health nutrition, including health worker training.
To date, the AIM Health Project initiatives have positively impacted 2,784 pregnant and lactating women and children under 5.
Empowered with knowledge, strengthened health systems, and community and family support, many more women in Esther’s community are breastfeeding their children longer and they can space their births adequately to greatly reduce the mortality rate. “Thank you, our lead mother, for always teaching and advising us,” says Esther. “We really appreciate your passion, personal sacrifices, and commitment to keep mothers and their children healthy and free from diseases.”
And now, Rogers has a dream for his twin daughter and son. “It’s satisfying to watch once tiny babies grow into bubbling human beings our twins are,” he says. “When they grow up, I want them to be just like the people from World Vision who helped us. I never knew there were such good people in the world. God bless your innermost heart desires.”
Rachel Auma, Monitoring and Evaluation Officer, Sophia Aloikin, Donor Liaison Officer and Fred Ouma, Development Communications Officer, World Vision Uganda