Saving babies born too early in Busia

Barbara, a 25-year-old mother, was excited about giving birth to her first child. She was happy about the good progress of her pregnancy.
“The early weeks of my pregnancy were fairly easy though I suffered a bit of nausea and fatigue occasionally,” says Barbara. “I attended my antenatal visits as advised by the health workers and the baby showed normal growth.”
In the 28th week, she started experiencing pregnancy complications with pain in her lower abdomen. She could hardly stand on her feet. While doing her normal chores, she lost consciousness and was rushed to a health centre.
“I was diagnosed with malaria and immediately put on treatment,” says Barbara. “Shortly after recovery, I started experiencing excruciating abdominal pain that resulted into labour pains. My husband rushed me to the same health facility and the doctor told me I was in labour.”
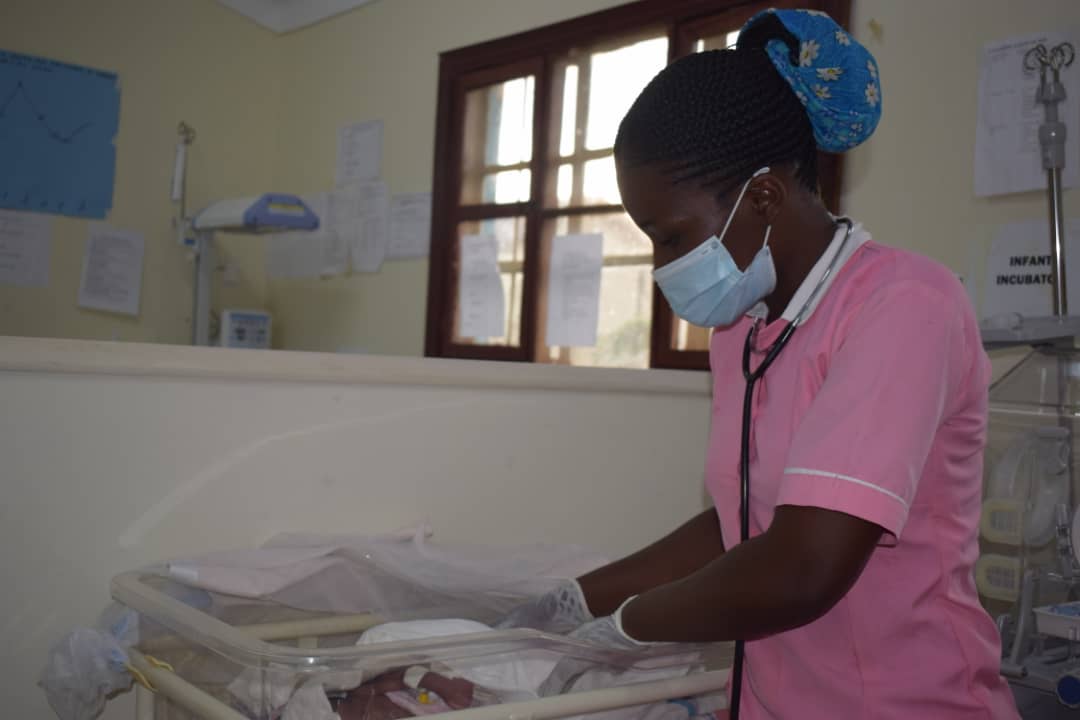
Shortly after, she had a normal delivery. After some time, they realised the baby had some complications and had trouble breathing and Barbara was referred to hospital. Thanks to World Vision and the Irish-funded project AIM Health, this hospital is equipped with a Neonatal Intensive Care Unit.
Her newborn baby, Favor, was introduced to Kangaroo Mother Care, where mothers use their body heat as a form of incubation for their premature child. With steady progress, the baby started to gain weight. Thirty days later, Barbara was discharged from hospital and asked to return for review in three days.
A ray of hope

World Vision, through the Aim Health Project, is restoring the hope and confidence of mothers by sustaining the wellbeing of neonates. Mothers like Barbara now have access to modern neonatal care equipment in health facilities that provide a stable environment for newborn babies.
The five-year project aims to reduce neonatal and under-five mortality rates by 20% and maternal mortality ratios by 15% between 2017 and 2021. The project currently operates in 16 sub-counties in Busia district, four of these are directly under World Vision Area Programmes.
According to the 2020 Uganda District Health Information system II, neonatal death in Busia district stands at 81 deaths per 532 pre-term births.
Aim Health Project Manager Mildred Orishaba says as of September 2020, out of 290 pre-mature babies born across the district, 270 survived. She attributes the high survival rate of pre-term babies to the training of health workers, renovations and equipping of health facilities in the district.
“Mothers in the district are now more confident even in situations where they deliver pre-term babies,” says Mildred. “This is largely attributed to the enhanced skills of health workers as well as equipping of the three high level facilities in the district with intensive care units.”
But it’s more than having the right equipment. It takes the right people with the right attitude and training. “The project continues to support the health facilities in managing of these cases but also ensuring that there is sufficient care provided to the mothers in the event that they come for services at the health facility,” she says.
The Hospital before intervention

Before World Vision intervened, the hospital registered high numbers of babies dying pre-maturely with late referrals being the major cause. The hospital lacked a postnatal corner and an intensive care unit for babies born before their term.
“Before the situation was worrying,” says Doreen Ntumba, a midwife at the hospital. “Now many things are have improved and continue to improve. As health workers we have been in various packages, including how to take care of babies born too early. In 2018, we even managed to set up a postnatal corner and designated a room as an intensive care unit for babies.”
The following year World Vision facilitated 10 more health workers from Busia district to attend a training on the management of newborn cases. Doreen was among the three health workers from the hospital.
After the training, a special room that had been designated as intensive care unit was equipped with beds, incubators, a phototherapy machine, an oxygen concentrator, a radiant monitor, and a pulsometer, and manned by qualified medical personnel.
As a result of this boost, Doreen says the hospital has witnessed an influx of people seeking health services. “We’re busier than ever,” she says. “On average we receive about 75 mothers for first antenatal care and deliver 66 women every month.”
“Thank you World Vision for choosing to work with us. Because of you, children like baby Favor are alive.”
Story by Racheal Auma and Sophia Aloikin, World Vision Uganda