Nutrition Basics
Nutrition Basics
Good nutrition is essential for infants and young children to grow, thrive, and live life to the fullest. A balanced intake of proteins, carbohydrates, fats, vitamins, minerals, and water is vital for healthy development and the proper functioning of body systems. When any of these nutrients are lacking, a child’s physical growth, cognitive development, and overall health can be seriously affected.
World Vision is committed to helping families and communities ensure every child receives the nourishment they need. Our programmes focus on tackling the most pressing global nutrition challenges, outlined below.
WHAT IS MALNUTRITION?
Malnutrition remains a critical global challenge affecting millions of children and families. It includes deficiencies, excesses, or imbalances in a person’s intake of energy and nutrients and can impact people of all ages.
TYPES OF MALNUTRITION
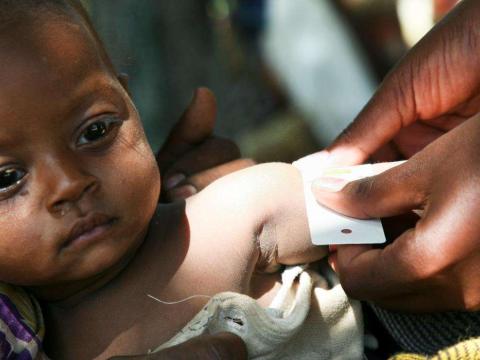
Stunting is when a child is too short for their age, indicating long-term nutrition deficiency (low height-for-age).
Wasting occurs when a child is too thin for their height, often due to recent and severe weight loss (low weight-for-height).
Anaemia: Iron deficiency is the most common micronutrient deficiency worldwide. Severe iron deficiency leads to anaemia - causing fatigue, reduced cognitive development, and weakened immune function. Millions of women, adolescent girls, and children are affected globally.
WHY ARE SO MANY CHILDREN MALNOURISHED?
Children face malnutrition for many reasons. These include poverty, conflict, displacement, and lack of access to diverse, nutrient-rich foods. Diets high in ultra-processed foods with low nutritional value, combined with poor water, sanitation, and hygiene (WASH), also play a major role.
WHAT ARE WE DOING?
World Vision implements a range of proven project models to deliver lasting nutrition impact, tailored to the unique needs of each community. Our approach addresses the root causes of malnutrition and empowers families to sustain healthy, well-nourished lives for their children.
Core Project Models
World Vision at the Nutrition for Growth Summit
World Vision's role at the Nutrition for Growth (N4G) Summit will include advocating for stronger nutrition commitments through our ENOUGH campaign to end hunger and malnutrition.